Scientists at Johns Hopkins are finding new ways to study Alzheimer’s disease without needing to look directly inside a patient’s skull. Instead, they are growing tiny, pea-sized clusters of brain tissue in a lab. These models, called organoids, are helping researchers understand why some drugs work for certain people but fail for others.
The team focused on the hindbrain, which is the part of the brain that handles basics like breathing and heart rate. Because Alzheimer’s affects more than 7 million Americans, finding a way to tailor treatments to the individual is significant. Currently, doctors often prescribe antidepressants like SSRIs to help with the anxiety and agitation that come with the disease, but these drugs don’t work for everyone.
Testing Alzheimer’s Treatments On “Mini-Brains”
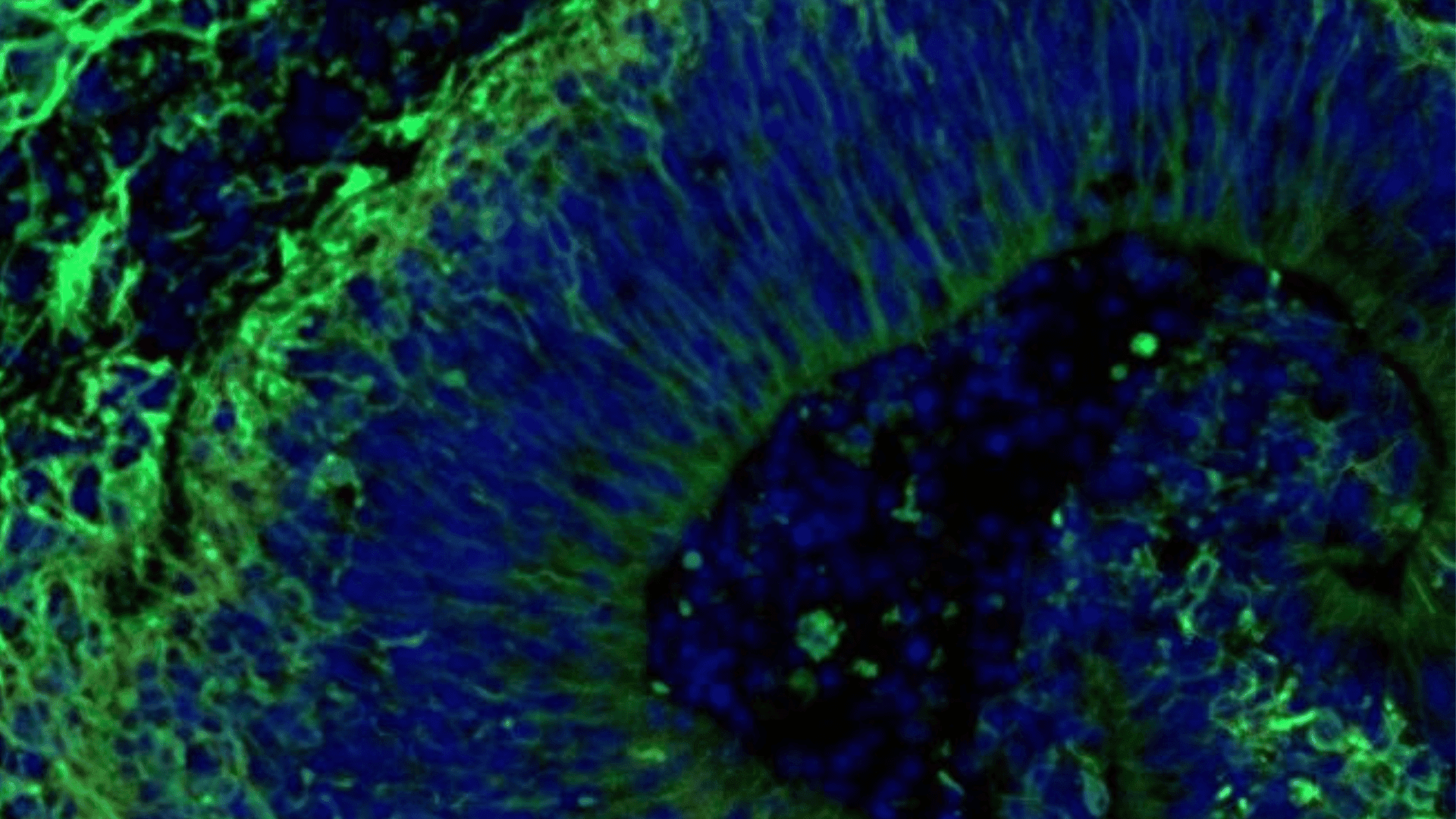

To build these models, researchers took blood samples from patients and turned those cells into stem cells. From there, they grew them into brain tissue that behaves like an actual brain. By creating hundreds of these organoids, the team could test how different people might react to a common antidepressant.
In some of the lab-grown samples, the drug worked well and boosted the proteins responsible for brain communication. In others, there was almost no change at all, suggesting that doctors might one day use these models to figure out which patients will actually benefit from a specific pill before they ever take it.
Advertisement
“Our study suggests that large-scale, patient-derived brain organoids and the vesicles they secrete can help us stage Alzheimer’s disease, investigate the mechanisms that drive it and assess how patient subgroups may respond to different treatments,” said study leader Vasiliki Machairaki, Ph.D.
Getting a Clearer Picture
The researchers also looked at tiny particles the organoids spit out, called extracellular vesicles. These particles carry a lot of information about what’s happening inside the brain cells. The team found specific protein changes that only show up in Alzheimer’s patients.
The hope is that these particles could act as a “liquid biopsy.” Instead of guessing how far the disease has progressed, scientists could look at these biomarkers to get a clear picture.
“We used these organoids to model how some patients’ tissue may respond to a commonly prescribed SSRI,” Machairaki said. “On a large-scale level, our model may eventually be used to identify subgroups of patients, based on underlying molecular mechanisms, who are more likely to respond to certain drugs and thus help us to create precise, targeted treatments in the long run.”
This isn’t the first study to explore lab-grown mini-brains, either. Researchers at the Paris Brain Institute are studying artificial brain tissue to help them understand child epilepsy.