Researchers at the Paris Brain Institute are testing lab-grown “mini-brains, to see exactly how the epilepsy condition starts.
Globally, approximately 50 million people suffer from active epilepsy. In France, around 700,000 people live with it. For many of them, medicine doesn’t help. This is often because of a brain malformation called FCDII, where nerve cells don’t organize correctly. In the past, the only real fix was risky surgery to remove the affected part of the brain.
Growing a Mini Brain
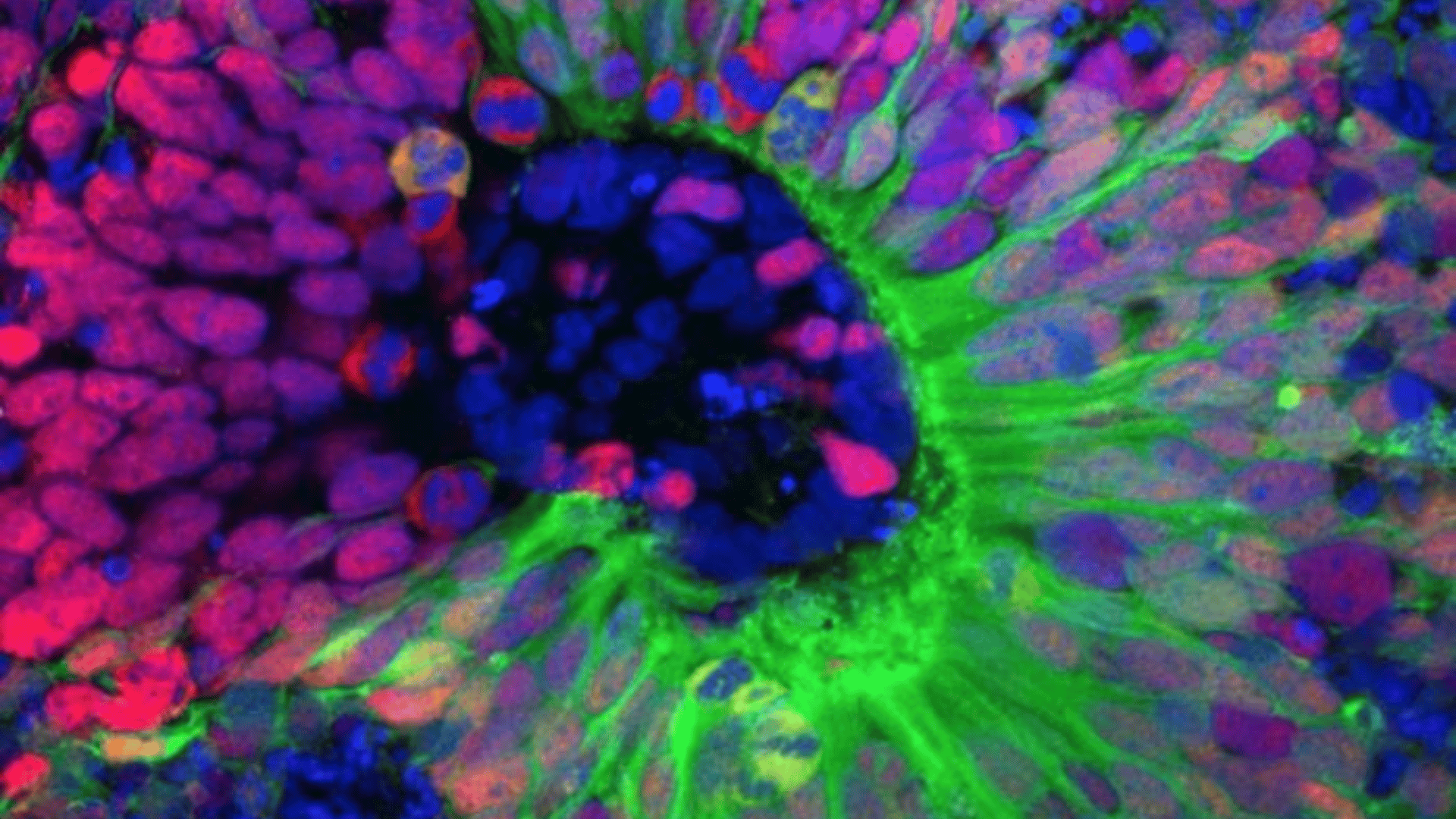

To get a clear picture, the team used blood cells from a young patient and his healthy brother. They turned these into stem cells and grew them into tiny models of the human cortex.
The researchers wanted to mimic a “mosaic” pattern. This is when some brain cells have a specific genetic mutation while others nearby stay healthy. They used a gene called DEPDC5, which is a big player in this type of epilepsy.
“Mouse models of this condition existed, but they didn’t fully capture the complexity of the human patients. Human cortical development has features you simply don’t find in mice,” says Marina Maletic, the study’s lead author. “So, we created human mosaic organoids by mixing cells carrying two mutated copies of the DEPDC5 with cells carrying only one. This allows us to recreate the genetic situation observed in patients’ brains.”
Advertisement
No More Surgery to Treat Epilepsy
By watching these tiny, 3D mini-brains grow for six months, the team confirmed a theory called the “two-hit” model. Essentially, you aren’t born with the disease just by inheriting one bad gene. You need a second, spontaneous “hit” to happen in a specific cell while the brain is still developing.
“A single inherited mutation in the DEPDC5 gene is not sufficient to cause FCDII. It is the acquisition of a second spontaneous mutation—in a specific cell, at a specific moment in brain development—that sets off the pathological process,” said Stéphanie Baulac, who heads the research team.
When that second hit happens, the brain gets “over-excited.” The researchers noticed that neurons in these models fired much more often than normal. While it isn’t a full seizure, it shows how the electrical balance in the brain breaks down.
“You can’t really talk about epilepsy in an organoid. It’s just a model, not a real patient! But we do consider this abnormal electrical activity to be a correlate of epileptic seizures in humans. It rounds off our description of the pathological process,” Maletic explains.
By finding these specific genetic triggers, the team hopes to find new ways to treat the condition without needing surgery.