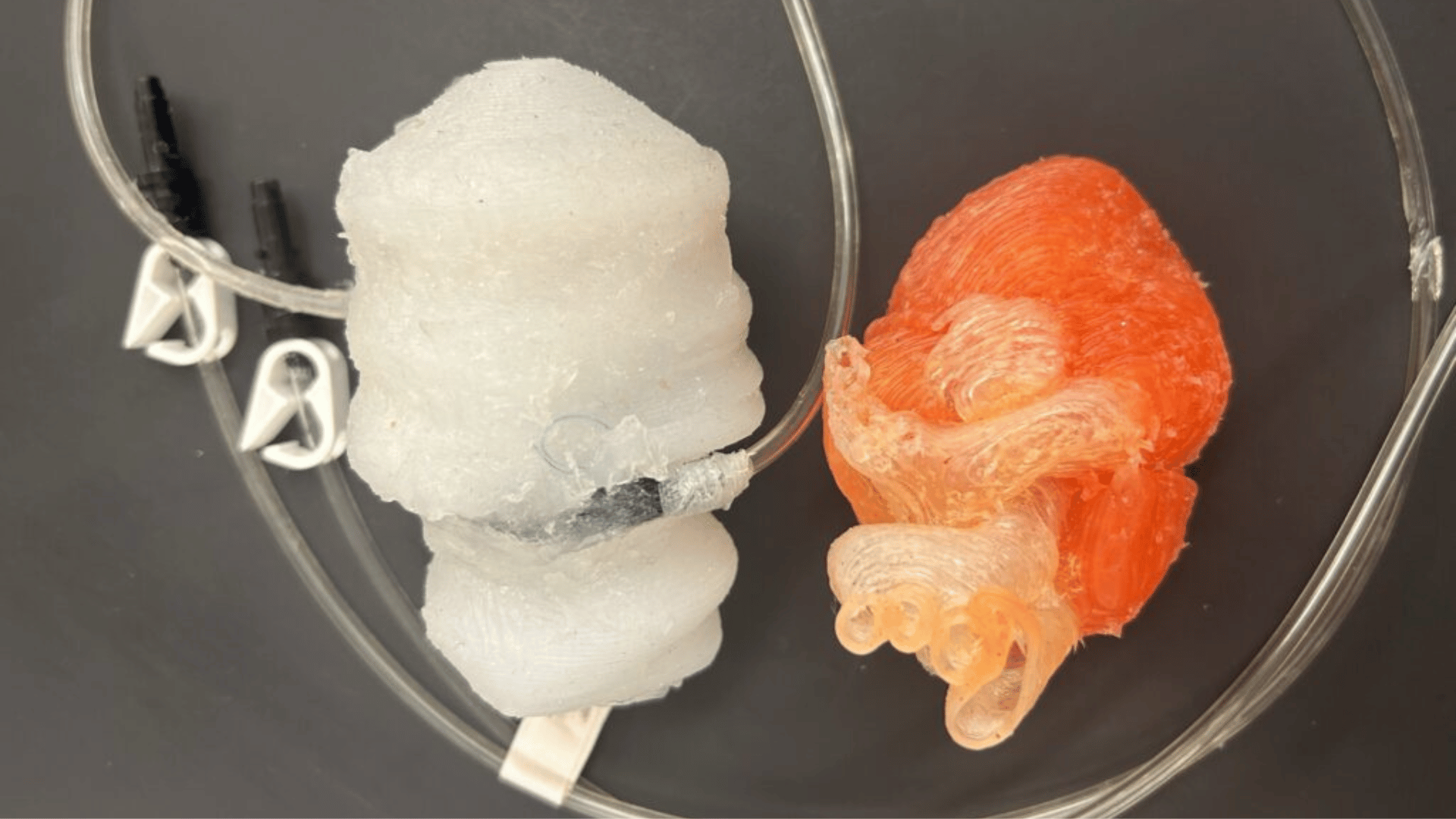
Researchers at The Ohio State University Comprehensive Cancer Center have found a way to potentially help patients with lung cancer who don’t respond to standard treatments like immunotherapy. Their study, recently published in Science Translational Medicine, looks at how cancer cells survive when we try to starve them of nutrients.
Breaking the backup plan

The team focused on non-small cell lung cancer (NSCLC). In the past, doctors tried to stop these tumors by targeting lysosomes, the tiny parts of a cell that act like a recycling center to keep the cell stable and fed. They used a drug called chloroquine to do this, but the results were often underwhelming. It turns out, cancer cells are good at finding a workaround.
The study found that when lysosomes are blocked, the tumor flips a switch on a protein called SREBP-1. This protein helps the tumor suck up more glucose, which gives it the energy to resist the treatment. It’s essentially a backup plan for the cancer.
“These findings reveal a previously unrecognized mechanism by which tumors withstand lysosomal inhibition, providing a strong rationale for combination strategies targeting lysosomal function alongside glucose and lipid metabolism to more effectively treat NSCLC,” said Deliang Guo, PhD, the study’s senior author. “This approach may also be applicable to other cancers with high metabolic demands for glucose and lipids that would present an even broader strategy for enhancing therapeutic outcomes.”
Advertisement
A New Path to Lung Cancer Treatment
By studying cell lines and animal models, the researchers showed that if you block that glucose transport at the same time you target the lysosomes, the tumor can’t cope. The cancer cells end up with damaged mitochondria and eventually die off.
“Our study is the first to reveal a previously unrecognized mode in which glucose and lipid metabolism are coupled to form a positive feedback regulatory loop,” said Dr. Guo. “This finding deepens our understanding of the regulation of complex metabolic networks in biological systems and uncovers the metabolic compensatory flexibility of tumors, as well as their ability to evade inhibition of a single metabolic node.”
Because some of the drugs used in this study, like chloroquine and simvastatin, are already approved for other uses, it might be easier to get these combination treatments to lung cancer patients who currently have few options.
“This study provides clear mechanistic guidance and a feasible drug-combination strategy to markedly enhance the antitumor efficacy of lysosomal inhibitors,” Yaogang Zhong, PhD, said.